But the increase marks good news for survival, study suggests
by Kristen Monaco, Senior Staff Writer, MedPage Today
Connect with Us:

But the increase marks good news for survival, study suggests
by Kristen Monaco, Senior Staff Writer, MedPage Today

This week, Senators on the Health, Education, Labor and Pensions (HELP) Committee have the opportunity to advance important legislation that supports rare disease innovation for children. Since 2012, the FDA has awarded companies that develop life-saving and novel therapies for children with rare diseases with priority review vouchers (PRVs) to help spur innovation in this critical area. The Give Kids a Chance Act (S. 932) would reauthorize the Pediatric Rare Disease Priority Review Voucher program through 2029. However, legislation extending this program must pass to ensure this important tool is reauthorized to address the significant unmet treatment needs that exist in the pediatric rare disease population does not end.

Living with Diabetes: Going the Distance
Zoe Heineman finished her fifth TCS New York City Marathon this past Sunday on November 3, 2019. The New York City Marathon course is tough even without a chronic condition like type 1 diabetes. This year more than 50,000 runners from all over the world took to the streets of New York City. Not everyone finishes! Even for elite runners, it is the most difficult marathon with hilly stretches over 26.2 miles. We got a chance to talk to Zoe about her success, endurance and courage.
Tell us about your first marathon?
In 2013, I was invited to accept a charity bib for the NYC Marathon by a non-profit I support. Entrance to the race included a training program. Although I had not run any distance longer than a 5k, the invitation appealed to me. I wanted to get in better shape and needed a challenge. The New York Marathon was a sort of a dream I had to do one day. It was an opportunity to train safely as part of a group of women with a coach in NYC’s Central Park, three mornings a week. I made a deal with myself that I wouldn’t try to prove anything out of pride, and that if at any point I became injured or stopped enjoying it, I would stop.
About a month before the day of the marathon I started to worry about what might happen if I had severe hypoglycemia out on the course. I contacted New York Road Runners (NYRR), who organized the event to request a running companion, such as a diabetes nurse or my nephew. NYRR told me I couldn’t pick just anyone I wanted, but they directed me to Achilles, who provides guides to athletes with disabilities. Achilles guides run with athletes in mainstream races, such as marathons and triathlons.
How hard is running with type 1 diabetes, honestly?
Running with type 1 diabetes is much harder than running before I was diagnosed with type 1 diabetes at age 24. If my glucose is high, my energy level is lower, and I get tired much more easily. Most of the time running drives my glucose lower, and therefore, I have to be prepared to stop and eat glucose until it goes back up to a safe level. Sometimes, unpredictably, it has the reverse effect. If my glucose spikes while running I usually keep going and take a little insulin if necessary.
I carry a bunch of stuff in a fanny pack which is a bit of a hassle, but it’s worth it to be able to run with peace of mind knowing that I am prepared for anything.
I believe that running has helped me become more in touch with my glucose levels and helped me reverse unawareness.
What do you carry when you run marathons?
For the marathon this year I carried:
Glucagon, Basqimi now that it’s available
Jelly beans in a plastic baggie
15 Gels (“Vanilla Accel” and “Maple Syrup Tap Endurance”)
Glucose meter
Lancet and landing device
Fast-acting insulin pen
Two pen needles
One Tru steel infusion set
Two alcohol swabs
Plus:
Hand warmers
Toe warmers
Phone in an arm band
Ear phones
iPod shuffle
Strips for the meter (I carried 18 strips with me, loose in my pack)
Like every day, I also wore my insulin pump that shuts off if I go below 75 mg/dl; my CGM, and a watch that keeps track of my pace and heart rate. I made a training playlist for each year that I have run the marathon. I play that in just one ear, on the left, so that I can talk with my guide who runs to my right.
How was the NYC marathon for you this year?
This year was an amazingly clear, sunny and cool weather day, which always helps. With diabetes, running in hotter temperature tends to drive my glucose lower. I felt great overall, feeling smart that I had rented a room in a hotel only 2 blocks from the bus I had to take at 5:15 am to the Runners Village. I always enjoy the crowds along the route, especially seeing the kids some of whom wear their Halloween costume for a repeat performance, and the people with funny signs like “This seems like a lot of work for a banana” and “You Run Better Than Our Government” and “Stamina Is Sexy” are some of my favorites. This year, there were 2 people dressed as Jesus, one running barefoot with a cross on his back. The other was along the route of mile 25 in Central Park, with a sign that read “The End is Relatively Near.” It is a rare view of the city only available to the marathon runners, from the 5 bridges you cross to the streets that on any other day are clogged in bumper to bumper traffic with honking horns.
When I see the Engineers Gate entrance to Central Park at East 91st and 5th Avenue, I suddenly realize the end really is near, and I have almost done it again. All my training and running has brought me to the point where I am about to finish the toughest marathon in the country, with the most uphill challenges. A warm wave of emotion that brings a tear to my eye, realizing that despite diabetes, or maybe because of the endurance I have built over the last 30 years, my body is able to do this. The mere fact that I’m able to run a marathon still astonishes me every time I cross that finish line. Timewise, my finishing time was 5 hours 57 minutes, only 22 minutes slower than my personal best of 5 hours 35 minutes in 2015. More importantly, to me, diabetes-wise, it was my best marathon ever, because I did not go below 92 mg/dl, and most of the race I stayed between 92-125. That is a huge improvement over past years, when my levels went as low as 45. I have never passed out during a run. I have passed out from a hypo a few times, but not since I started running. I believe that running has helped me become more in touch with my glucose levels and helped me reverse unawareness.
What’s next?
Next year is the year of Vision, 2020, and I have decided to celebrate my good vision by participating in 20 running or triathlon events, including of course, the 50th anniversary of the New York City marathon on November 1, 2020. If you want to join me, I invite you to join Achille International and start working out with us on Tuesdays at 6pm and Saturdays at 10am in Central Park Contact Michael Anderson with any questions manderson@achillesinternational.org or visit http://www.achillesinternational.org to find a chapter near you.
When Zoe is not running, she works for Oxurion, NV, a Belgian biopharmaceutical developer dedicated to helping people with retina conditions preserve their vision. Also, Zoe started a not-for-profit initiative called Ha! short for Hypoglycemia Awareness, whose mission is to train First Responders to recognize and respond to the symptoms of severe hypoglycemia in public.
Share this:
Click to share on Facebook (Opens in new window)Click to share on Twitter (Opens in new window)Click to share on LinkedIn (Opens in new window)
Elizabeth Snouffer is Editor of DiabetesVoice.org
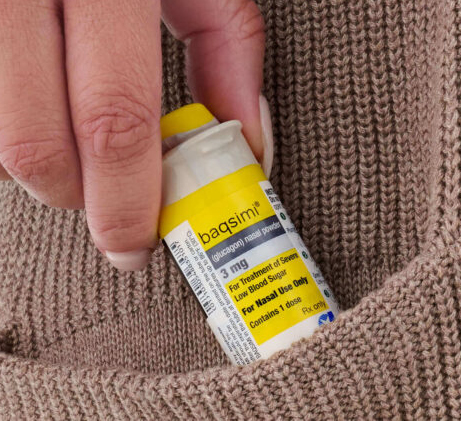
Baqsimi, the nasal glucagon available from Lilly is available. Although it is super easy to use, it’s completely new and different from other products you have encountered with diabetes management . Click on the link below to watch a video and learn how Baqsimi works before you and your friends, family, caregivers and co-workers need to use it. Be prepared for Baqsimi.
https://www.baqsimi.com/how-to-use-baqsimi
A few weeks ago, I found myself in a situation that required the use of Baqsimi. Although I had read the instructions, I had not watched the video, and wish that I had done so in retrospect. The product is very easy to use, but a video is always nice to watch before using something as important as this for the first time.
The website for Baqsimi is nicely presented, and has some support for people with diabetes who need help getting it. Here is a link for information that can lower the copayment to 0 for qualifying persons through December, 2019:
https://www.baqsimi.com/patient-support
I carried Baqsimi glucagon with me in my SPI belt during the NYC marathon last Sunday, and thankfully I did not need it. Just having it handy gave me peace of mind. It is only a few inches long and fits in the palm of your hand.

Hypos happen everywhere, and thankfully STARBUCKS are everywhere, so it’s helpful to remember that there are honey packets at the condiment station, just in case you have a hypo moment while you are enjoying your beverage. It probably wasn’t intended to be used as a mini rescue for hypoglycemia by Starbucks management, but I for one am delighted to have them available when and if I am out and about in the city, running and need to replenish the glucose level or gel packets in my SPI belt. Sometimes all you need is a honey packet. I have kept leftover honey packets in pockets for months without any trouble and even put some through wash cycles without them breaking open. Here is a quick video to show you where to find the honey packets at Starbucks.

Big news at ADA 78th Scientific Sessions this year was the FDA approval of Senseonics’ Eversense device: the first implantable Continuous Glucose Monitor. The featured picture here shows where the on-body transmitter is worn by a gentleman who has been using it for 180 days in Germany. Fewer start-up days, less down-time and higher rate of accuracy are some of the advantages shown in the clinical trial, when compared to other CGM devices. People who prefer not to have to insert something into their skin themselves will be pleased to know that the insertion of a tiny sensor is performed entirely by the physician in a 10-minute outpatient office procedure. Here’s a 2 minute video showing how it works: https://www.eversensediabetes.com/eversense-cgm-system/
The sensor is about half the length of a match and about as big around. Training and certification for the physician is scheduled and performed by Eversense staff at the physician’s office. Users need to return to the physician’s office every 90 days to get the sensor exchanged for a new one in the opposite arm. The user who spoke at the product theater presentation for Eversense mentioned that he has already worn the system during several marathons and triathlons with greater peace of mind and no technical issues. He likes the unobtrusive, quiet, on-body vibration that alerts him to changing trends in his blood glucose patterns. His family and friends also like it because it gives them greater peace of mind so much that they almost forget he has diabetes.
Eversense will be taking its “Ever Mobile” lab unit across the country to introduce the technology to health care professionals. “Research has repeatedly demonstrated the clinical benefits patients experience with regular CGM use, including improved glucose control and protection against severe hypoglycemia,” said Steven Edelman, MD, @TCOYD Professor of Medicine at University of California San Diego, Founder & Director of Taking Control of Your Diabetes, and Senseonics Board member. “Despite these benefits, a significant number of people with diabetes do not use, or have access to, continuous glucose monitoring. Furthermore, the data shows that many people who’ve tried traditional CGM in the past either don’t wear it as often as they should or don’t stick with it for a variety of reasons, including concerns surrounding sensor accuracy, sensor insertion, and sensor discomfort. So, it’s important that patients have choices and that medical device companies continue to advance the field of CGM with innovations that make it easier for the end user.” In this really great video, Dr. Edelman outlines the benefit of this for people with type 1 and type 2 diabetes:
It is wonderful to have more choices for patients, which will lead to greater acceptance of CGM technology and better blood glucose control. Less hypoglycemia, more time in range = more you.

Starting a new school year is a logical time for people who have diabetes to get in the habit of refilling their prescription for glucagon (see example below), and used the expiring kit to train the people around them how to use it. Students and their parents, need to train teachers and school nurses. Coaches and childcare providers also need to be trained how to use Glucagon kits in case of severe hypoglycemia. Fellow classmates need to be trained how to recognize when help is needed to call an adult. Anyone who might be a first responder to someone with diabetes could help. To learn more, watch Safe at School: Chapter 6 – Glucagon Administration – YouTube 
In order to learn from each other’s experience, I am gathering anecdotes and stories around hypoglycemia during September which is Hypoglycemia Awareness month. Today I invite you to share a story of your own regarding an episode of severe hypoglycemia. Please send them to me directly via email to hoyzoya@gmail.com I will be posting what you share, and keeping them anonymous.
Thank you for reading. Thank you for your always welcome comments and contributions that guide me in knowing what you think and feel about the topics I raise.